About the Bundle
The national maternal safety bundles have primarily been focused on the inpatient setting. Recognizing the need to extend these protections beyond the hospital, this work has been adapted as the “Outpatient Severe Hypertension Bundle”.
About This Tool
We have studied this tool extensively and have adapted it across several contexts to best meet the needs of our users.
How to Use This Website
This website provides resources and guidance to support maternal safety practices. Here you will find evidence-based bundles, educational materials, and implementation tools to help improve outcomes. Below you will find that we have adapted these materials in a Clinical Practice Bulletin for the outpatient setting:
Readiness
Having the systems, protocols, and teams in place before a crisis occurs. Every outpatient care setting should establish the foundational processes below.
What is readiness?
How to use this section
What you will find in this section
Resources and materials designed by our team to support readiness implementation.
Recognition & Prevention
Every Patient:
- Ensure accurate measurement and assessment of blood pressure for every pregnant and postpartum patient, including via home blood pressure monitor if indicated.
- Screen for structural and social drivers of health that might impact clinical recommendations or treatment plans and provide linkage to resources that align with the pregnant or postpartum person’s health literacy, cultural needs, and language proficiency.
- Provide patient and support person education, including culturally appropriate resources and printed materials, on early warning signs of severe hypertension/pre-eclampsia and how to get help.
- Provide ongoing education to all health care team members on the recognition of signs, symptoms, and treatment of hypertension.
Recognition & Prevention Resources
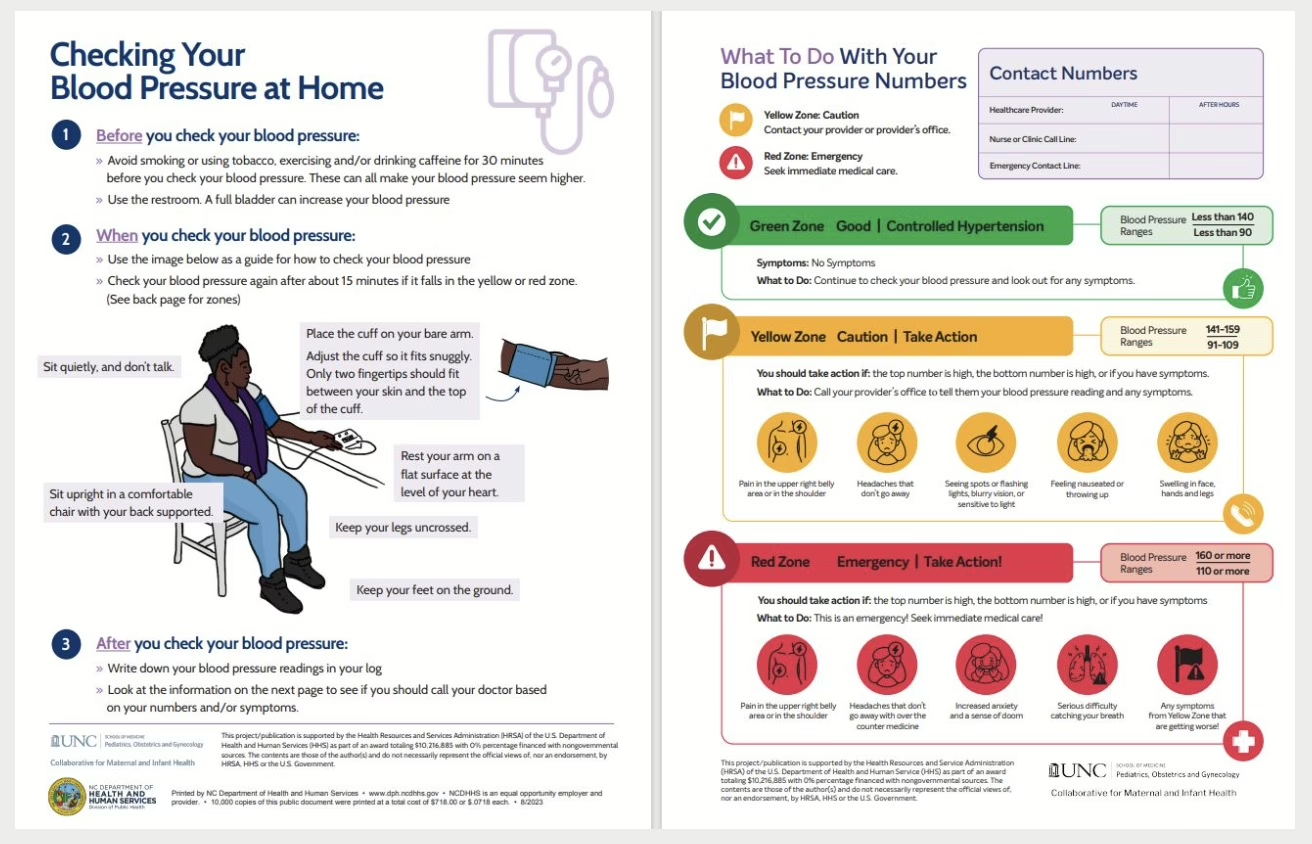
- Checking Your Blood Pressure at Home and What to do with your Blood Pressure Numbers English, Spanish Version
- CDC HEARHer for Partners, Friends and Family of Pregnant or Postpartum Women
- Blood Pressure Log for Patients
- The Maternal Early Warning Criteria
- AIM Maternal Early Warning Criteria (coming soon)
- CMQCC Preeclampsia Early Recognition Tool
Response
Every Case of Severe Hypertension:
- Utilize standardized protocols with checklists and escalation policies including:
- A standard response to maternal early warning signs
- Listening and investigation patient-reported and observed symptoms.
- Evaluation and management of episodes of severe hypertension/pre-eclampsia during pregnancy and postpartum
- Minimum Requirements for Protocol
- Notification of provider if systolic BP =/> 160 and/or diastolic BP =/> 110 (severe range) and retake in 15 minutes
- After the second severe range BP, treatment with oral Nifedipine IR (10 mg) should be initiated if available (ASAP, ideally within 30 minutes of BP verification)
- Escalation and care transition
- Maternal transport (algorithm) [Clinic Specific]
- Provide trauma-informed support for patients, identified support network, and staff for serious complications of severe hypertension, including discussions regarding birth events, follow up care, resources, and appointments.
Response Resources
- Outpatient Severe Hypertension Evaluation and Management
- Treatment of Severe Range Blood Pressure Algorithm
- ACOG Maternal Safety Bundle for Severe Hypertension in Pregnancy (See slide 29)
- OB Hypertensive Emergency Nifedipine Task Checklist
- ACOG Article: Postpartum preeclampsia or eclampsia: defining its place and management among the hypertensive disorders of pregnancy
- Case Study: Preeclampsia with Severe Features in the Outpatient Setting
- O-HTN-BP-1-Scenario-1
- O-HTN-Support-Person-Scenario-1
Reporting & Systems Learning
Every Clinic:
- Establish a culture of multidisciplinary planning, huddles, and post-event debriefs for every case with severe hypertension/preeclampsia (include the patient and support person when feasible) to identify successes, opportunities for improvement, and action planning for future events.
- Perform multidisciplinary review of all severe hypertension/pre-eclampsia cases to identify systems issues.
- Monitor outcomes and process metrics related to severe hypertension disaggregated by race and ethnicity.
Reporting Systems/Learning Resources
Respectful, Equitable & Supportive Care
Every Team Member/Every Clinic:
- Engage in open, transparent, and empathetic communication with pregnant and postpartum people and their identified support network to understand diagnoses, options, and treatment plans.
- Include pregnant and postpartum persons as part of the multidisciplinary care team to establish trust and ensure informed, shared decision-making that incorporates the pregnant and postpartum person’s values and goals.
- Ensure all educational resources and printed materials are appropriate for the patient’s health literacy, cultural needs, and language proficiency.
- Assess patient and support person’s understanding of the urgency of timely treatment of severe hypertension and escalation of care.
- Acknowledge patient’s concerns and assist with overcoming obstacles to going to the hospital (e.g., childcare, financial stress, past hospital-related trauma, etc.) and care plan (medication, appointments, antenatal testing).
- Implement strategies to mitigate racial/ethnic disparities identified through data collected.
Respectful, Equitable & Supportive Care Resources
Practice Bulletin References
Hypertension Practice Bulletin Resources References:
- MSc JEM, Mph AVM, Pettker CM, Simhan AH. Gestational Hypertension and Preeclampsia: ACOG Practice Bulletin, Number 222. American College of Obstetricians and Gynecologists. 2020 Jun 6;135(6): e237–60.
- Paul G. Schmitz TN. Hypertension, Clinical Updates in Women’s Health Care. American College of Obstetrics and Gynecology. 2016
- AIM PATIENT SAFETY BUNDLES [Internet]. ALLIANCE FOR INNOVATION ON MATERNAL HEALTH. 2021. Available from: https://saferbirth.org/psbs/severe-hypertension-in-pregnancy/
- Pregnancy Mortality Surveillance System [Internet]. CDC Centers for Disease Control and Prevention. 2022. Available from: https://www.cdc.gov/reproductivehealth/maternal-mortality/pregnancy-mortality-surveillance-system.htm
- Howell E et al. Reduction of Peripartum Racial and Ethnic Disparities: A Conceptual Framework and Maternal Safety Consensus Bundle. Journal of Midwifery & Women’s Health. 2019 May;63(3):353.
- HEAR HER Campaign [Internet]. CDC Centers for Disease Control and Prevention. 2022. Available from: https://www.cdc.gov/hearher/index.html
- California Collaborative on District Reform. Available from: https://cacollaborative.org/


